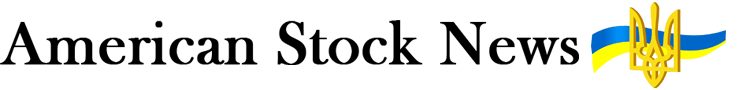She had driven herself to the emergency room at Corona Regional Medical Center on a blistering afternoon in July. She was 38 years old, 30 weeks pregnant, and she could not breathe.
Ramirez woke up from a medically induced coma nearly three weeks later. In a different city. In a different hospital. Hooked up to a ventilator. The room was dark. Her first thought? That she had somehow ended up in a dungeon. And then she heard
“All the doctors and nurses were clapping and high-fiving,” she said. “They were asking my nurse for the day, ‘Where’s her baby? How’s her baby?’
“But I didn’t know what baby they were talking about, because I was still pregnant.”
The jubilation in the intensive care unit at Loma Linda University Medical Center that day stemmed from a simple fact: Ramirez had regained consciousness. Fourteen days earlier, doctors had delivered her baby by emergency caesarean section.
Emiliana was born July 13 — 10 weeks early, weighing 3 pounds, 6 ounces. She needed a ventilator for the first several days of her life. More than a month would pass before she felt her mother’s touch. She spent her first eight weeks in the neonatal intensive care unit.
The day Ramirez delivered Emiliana, the new mom was one of 19,502 people in hard-hit San Bernardino County who had contracted COVID-19. (The county has now reported more than 61,000). She was one of 616 confirmed cases in a hospital there and one of 174 in a San Bernardino County intensive care unit.
Of the 48 pregnant women who have been admitted to Loma Linda University Medical Center with COVID-19, 45 are Latina — an extreme snapshot of a disease that has infected and killed Latinos at a rate disproportionate to their share of the population.
Very little is known about the impact of COVID-19 on women and the babies they carry. It is still not clear how a pregnant woman passes the virus on in the rare cases in which a baby has become infected. Most of the early research on COVID-19 has used data from older men, because they have gotten sickest and died in greater numbers.
“What’s unique about COVID-19 is we haven’t really been able to identify out of the gate why some moms seem not sick at all,” said Dr. Courtney Martin, medical director for maternity services at Loma Linda University Children’s Hospital. “And then another portion are insanely sick, like Monica. Who almost died. Several times.”
Experts are learning more every day about the new coronavirus that causes COVID-19. The American College of Obstetricians and Gynecologists (ACOG) is following the situation closely. This page will be updated as ACOG learns new information for pregnant and breastfeeding women.
Researchers are still learning how COVID-19 affects pregnant women. Current reports suggest that pregnant women may have a higher risk for more severe illness from COVID-19 than nonpregnant women. Reports note that:
- Pregnant women with COVID-19 may be more likely than nonpregnant women with COVID-19 to need care in an intensive care unit (ICU) or need a ventilator (for breathing support).
- Pregnant women with some health conditions, such as obesity and gestational diabetes, may have an even higher risk of severe illness, similar to nonpregnant women with these conditions.
- Pregnant women who are Black or Hispanic have a higher rate of illness from COVID-19 than other pregnant women. But it’s not about biology. Black and Hispanic women face social, health, and economic inequities that put them at greater risk of illness. To learn more about these inequities, see this page from the Centers of Disease Control and Prevention (CDC).
Also, it’s important to know that reports suggest the risk of death is not higher for pregnant women with COVID-19 than for nonpregnant women with COVID-19.
How can COVID-19 affect a fetus?
Remember that researchers are learning more about COVID-19 all the time. Some researchers are looking specifically at COVID-19 and its possible effects on a fetus. Here’s what they know now:
- Researchers have found a few cases of COVID-19 that may have passed to a fetus during pregnancy, but this seems to be rare.
- Researchers have studied COVID-19 infection, preterm birth, and stillbirth. Some studies suggest there may be an increased risk of preterm birth and stillbirth for women with COVID-19. Other studies have not found this to be true. But information is still limited. Researchers are continuing to study these outcomes to better understand the effects of COVID-19 before birth.
After birth, a newborn can get the virus if they are expose
Pregnant women can stay healthy by following the usual recommendations during pregnancy, including:
- Eating healthy meals (see Nutrition During Pregnancy).
- Exercising regularly (see Exercise During Pregnancy, though be mindful to stay at home or away from other people while exercising).
- Getting plenty of sleep.
- Avoiding alcohol and drugs (see Tobacco, Alcohol, Drugs, and Pregnancy).